A) Runny noses are tricky. On one hand, they’re a common symptom of COVID-19. On the other hand, they are usually due to some other bug.
Getting tested is the only way to know for sure what you’ve got. Whether or not you test, be kind and spare others not just from the sniffles, but also the stress they bring.
Here’s the TL;DR on the runny nose paradox:
How often do kids with COVID-19 have a runny nose?
👃🏻Runny noses are one of the most common symptoms of COVID-19 in kids. A large UK study of kids with symptomatic COVID-19 found runny noses in roughly 50% of older kids and 40% of younger kids. In some cases, a runny nose is the only symptom, though other symptoms often follow. A community study in Canada reported that 1 in 25 kids with COVID-19 had a runny nose as their only COVID-19 symptom.
📊Check out the figure for the scoop on COVID-19 symptoms in kids, and don’t forget that up to half of kids show no symptoms at all (excluded from this study).
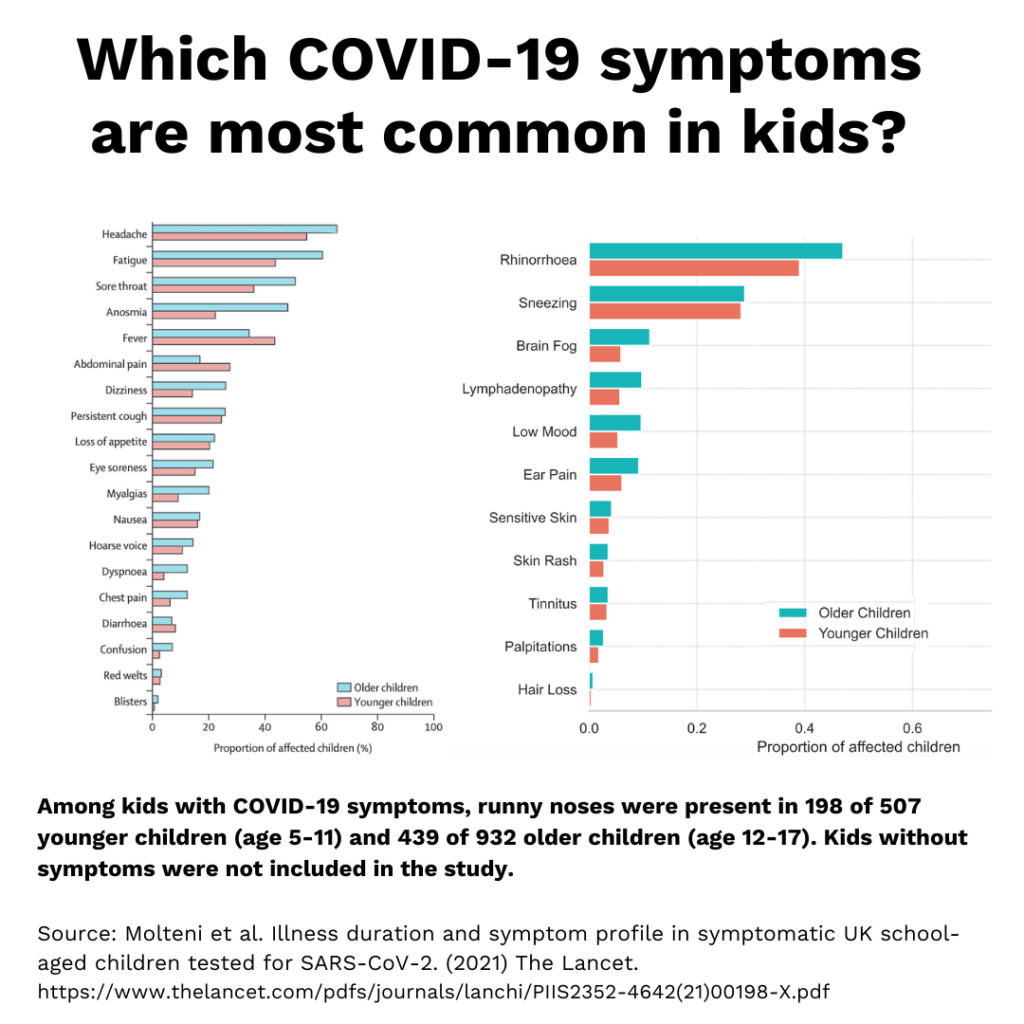
*Note: It’s too early to know if these numbers are different for the delta variant as it takes months to complete and publish scientific studies.
How well do runny noses predict COVID-19?
😮💨Thankfully, most cases of sniffles in kids are just colds, not COVID-19. This doesn’t mean that testing runny noses is pointless, just that we may have to test many sniffy kids to catch a case of COVID-19. This metric of test value, called “Number Needed to Test” can change radically depending on who is being tested, and in what context.
For example, a Canadian study estimated that you’d catch one COVID-19 case if you tested 15 primary kids with runny noses as their only symptom, among those with a known high-risk exposure.
To catch a COVID-19 case among older kids in the same boat, you’d only need to test 6 of them.
⭐The likelihood that your sniffly child tests positive depends on three things: their other symptoms (if any), their COVID-19 exposure risk, and the chances that their sniffles have another explanation.
🤒The value of testing skyrockets if your child has multiple symptoms, especially if they include symptoms that are more specific to COVID-19, like loss of smell or taste, nausea/vomiting, headache, and fever.
🦠A sniffle-induced COVID-19 test is more likely to come back positive if your child lives in a COVID-19 hotspot, or has a known high-risk exposure.
🤧The value of testing runny noses tends to increase as kids get older, and less … snotty.
Similarly, testing delivers less bang-for-the-buck during cold and flu season than the rest of the year.
Testing Tips
🧪A COVID-19 test is the only way to be sure what you’re dealing with. If you have access to testing, take advantage, the sooner the better. Both PCR and rapid antigen tests perform best in the first few days of symptom onset.
👩🏽🔬PCR testing is the gold standard, but rapid antigen testing once a day for 2-3 days after symptom onset is almost as good as PCR. If multiple family members have a runny nose, rapid test everyone for a confident answer.
🤓Nerd Note: Public health policies for testing runny noses are all over the map. In some places, a runny nose is enough to trigger testing. In others, a runny nose doesn’t make the cut for school health screening. Local policies reflect differences in testing resources and prioritization, not scientific debate on the link between runny noses and COVID-19.
The Bottom Line
🧘🏽If your kid has a runny nose, don’t panic, but do take action. If you have access to testing, use it – especially in older kids, or when exposure risk is high. Every COVID-19 case that we catch has a huge impact on families and communities.
🏠Regardless of whether you test, protect others by keeping your sniffles at home. A simple runny nose can wreak havoc these days!
⚠️This advice should not supersede your local public health recommendations.
Thanks!
🙏Thanks to Chana Davis, PhD of Fueled by Science for this post. Chana is currently recovering from a runny nose (COVID-19 negative, phew!).
DP links
Should I take a COVID-19 rapid antigen test? Part 1 in a Series
Should I get tested after X (fill in the blank)? Part 2 in a Series
I’ve been exposed to COVID-19! When should I get tested?
Do you have practical advice for families around testing for COVID-19?
How will I know if my symptoms are from the flu or covid-19? If I am not sure, what should I do?
Studies
Illness duration and symptom profile in symptomatic UK school-aged children tested for SARS-CoV-2
Predicting SARS-CoV-2 infections for children and youth with single symptom screening


