A: The best time to test for COVID-19 depends on your situation.
NOTE: Updated for clarity on 2/8/22
➡️ If you were exposed, the sweet spot to test is 3-5 days later*
➡️ If you develop symptoms, test right away*
➡️ If testing to leave isolation, check for a negative rapid test on day 5 (US guidance)
➡️ If testing before an event, test as close to the event as possible.
*A follow-up test may be needed in 1-2 days to reduce false negatives.
TL;DR. A typical COVID-19 infection progresses from exposure, to incubation, to symptoms, to viral clearance. Yet, the timing of these phases varies greatly across variants and people (see figures).
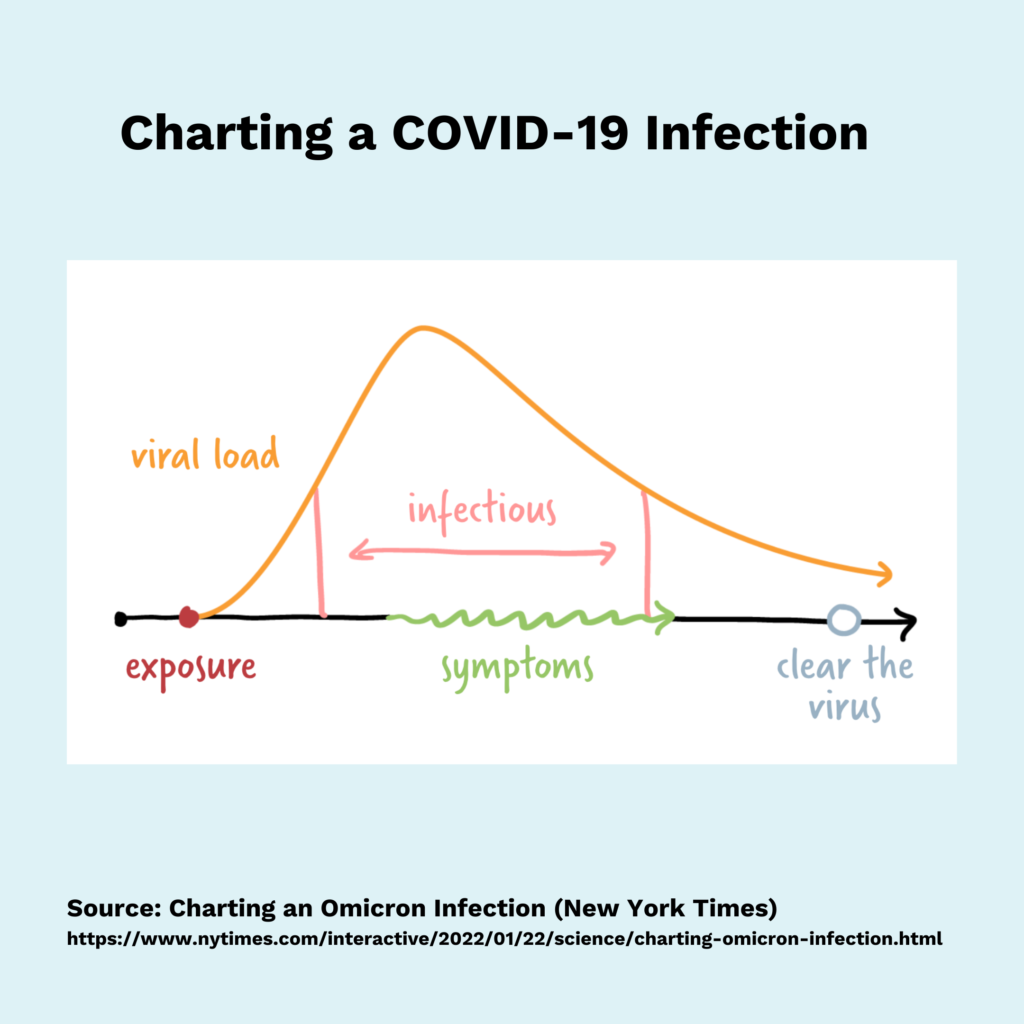
While science can’t predict the precise moment you will test positive, it can provide a rough window for testing, and help you make sense of your results. Your optimal testing strategy should also consider test access, turnaround time, and how test results will impact your choices.
🧪PCR vs Rapid Antigen Tests: Rapid tests are only positive during the peak infectious period because they require lots of viral protein to light up. PCR tests, which detect tiny bits of viral RNA, are far more sensitive. They typically catch an infection a day or so before rapid tests, and can stay positive for weeks after the infectious period is over.
 Where to swab? Growing evidence suggests that dual throat/nose swabs are better than nasal swabs for Omicron. Also, saliva PCR may catch cases a bit earlier than nasal PCR.
Where to swab? Growing evidence suggests that dual throat/nose swabs are better than nasal swabs for Omicron. Also, saliva PCR may catch cases a bit earlier than nasal PCR.
Here are some guidelines to help you chart your course:
IF YOU WERE EXPOSED
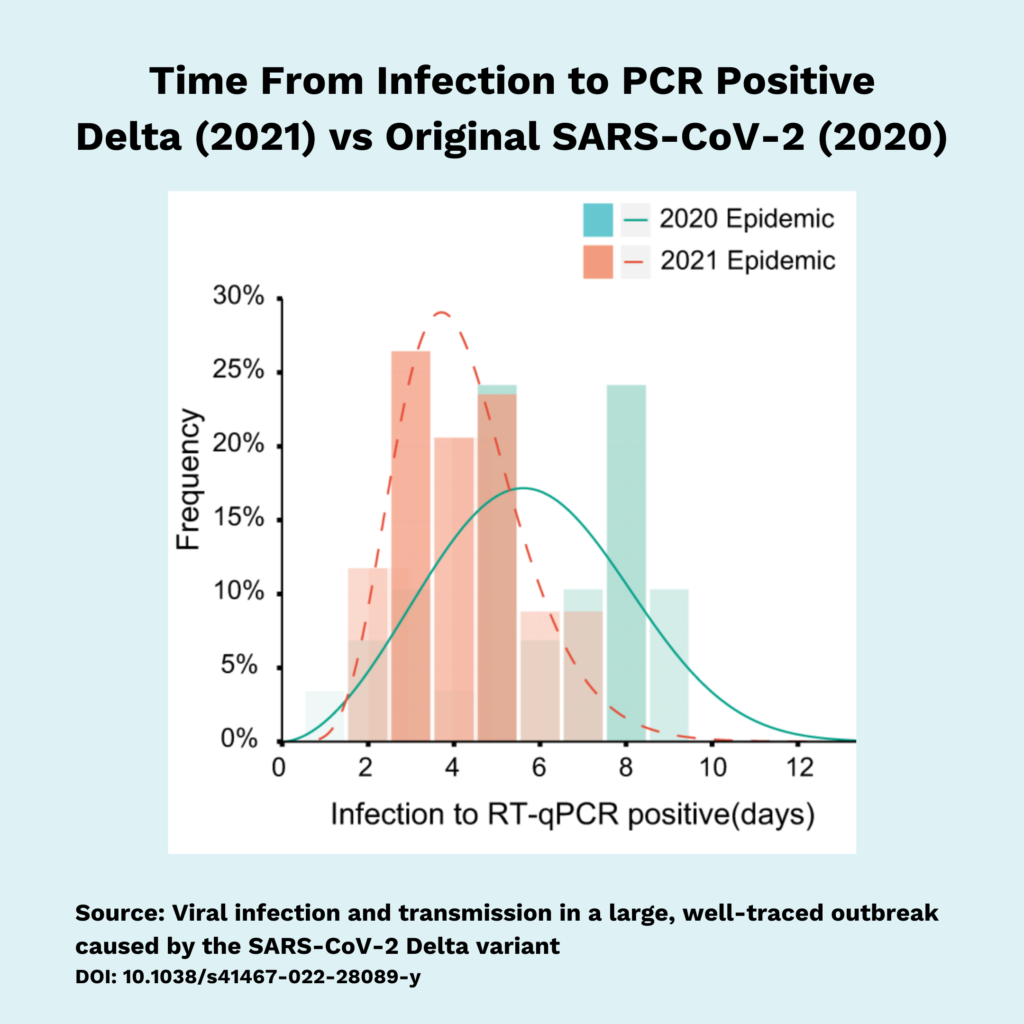
The US CDC recommends waiting at least 5 days after exposure to test, to maximize the odds that the virus has replicated to detectable levels. That said, many Omicron cases are detectable 3 days after exposure by PCR or rapid testing, and some as early as 2 days after exposure.
If you opt to test early (before Day 5) bear in mind that even PCR can give a false negative at this point. It may be that the virus didn’t take off and start making lots of copies YET. If an early test is negative, test again 2 days later to rule out an infection. After a full 5 days, we can be much more confident in a negative test result. Always take precautions while your COVID status is uncertain.
IF YOU DEVELOP SYMPTOMS
The U.S. CDC recommends testing (with either a PCR or rapid test) as soon as you have symptoms. When symptoms are present, PCR performs very well and can catch the vast majority of cases. Rapid tests are less reliable immediately, and can take a few days before they turn positive, especially with Omicron.
If you are using rapid tests, and have only one, consider waiting 2-3 days after symptoms to reduce the chances of a false negative test result. Otherwise, use one test immediately upon symptom onset, and save the other for a re-test in 2-3 days. In the early days, you can trust a positive rapid test, but not a negative one. Take precautions and isolate yourself from others until you can rule out COVID-19.
⚠️ Don’t wait too long! Viral levels often drop substantially after the first week of symptoms and may no longer be detectable by rapid tests (though likely still by PCR).
IF YOU ARE IN ISOLATION WITH A CONFIRMED INFECTION
The U.S. CDC guidelines include an optional rapid antigen test after 5 days of isolation. If your test is negative, you no longer have to stay home, but should continue to wear a high quality mask around others until after day 10. If your test is positive, you can either continue to isolate for 5 more days or try again for a negative rapid test every 1-2 days.
For most people, it takes 5-10 days to clear enough virus to test negative on a rapid test, though it can take considerably longer for those with severe disease or compromised immune systems. A recent study of the Omicron variant in the National Basketball Association found that in half of players, their viral load had fallen from high to moderate after Day 5, while the other half were still teeming with virus beyond this point.
It’s worth noting that isolation policies differ around the world. The UK requires two consecutive negative rapid antigen tests, a day apart, with the first test no sooner than Day 5 (in England).
⚠️ PCR tests should not be used to determine whether you should end isolation, because they can be positive for weeks to months after the infectious period.
BEFORE A GATHERING
Test with a rapid test as close as possible to the gathering for your best chances of catching an infection and sparing others. Fair warning, some early infections can slip through the cracks as virus levels may be too low to be picked up by a rapid test at the time you take the test, even though you are infected. Rapid testing is therefore a powerful layer of protection but is not foolproof.
Keep calm and test on!
Thanks to Nerdy Girl Dr. Chana Davis (FueledbyScience) for keeping on top of the evolving science of testing!
Dear Pandemic Links
UPDATE on detecting Omicron with Rapid Antigen Tests
Does a positive COVID test mean that I’m contagious?
References
Charting an Omicron Infection (New York Times)
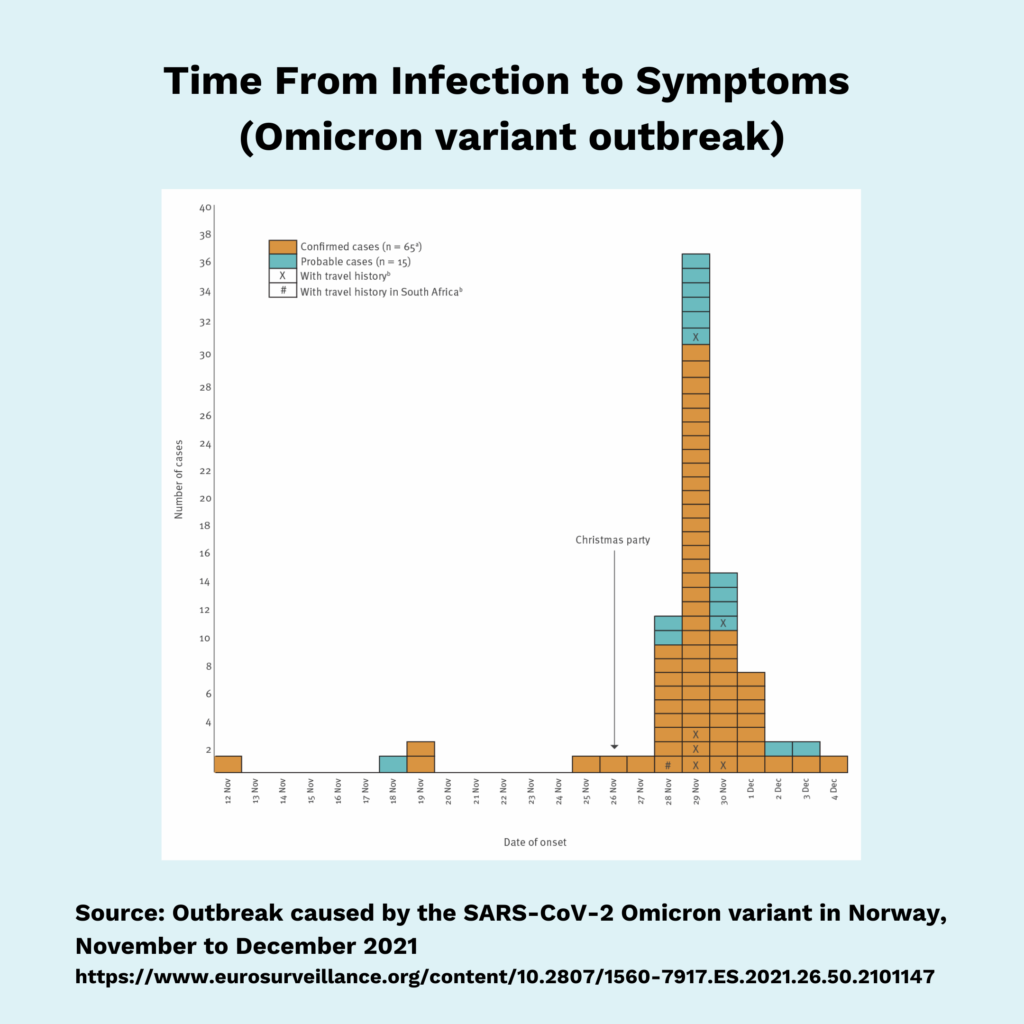
Outbreak caused by the SARS-CoV-2 Omicron variant in Norway, November to December 2021
Viral dynamics and duration of PCR positivity of the SARS-CoV-2 Omicron variant (preprint, not peer reviewed)
Discordant SARS-CoV-2 PCR and Rapid Antigen Test Results When Infectious: A December 2021 Occupational Case Series (preprint, not peer reviewed)



